DCS
The Early Days of Technical Trimix Diving
The use of trimix, that is a breathing mix of oxygen, helium and nitrogen has become the standard for dives beyond 30-50m/100-165 ft, depending on who you dive with. However, things were much different when mixed gas technology was just emerging. Here is an in depth look at the early days of what was then called “special mix” diving including an explanation of special mix tables by Dr. RW Bill Hamilton, a report on the first 1500 trimix dives by then aquaCORPS chief Michael Menduno, and a selection of Key West Diver Consortium tables for dives to 76 m/250 ft. From the aquaCORPS archives.

Reports by Michael Menduno and Dr. RW Bill Hamilton
Header image: Jim King and his team including Dustin Clesi and Larry Green prepare for a dive at Diepolder 1993. Photo from the aquaCORPS archives
Stories in this section:
Is The Market Ready for Mix? aquaCORPS Editorial by Michael Menduno, 1992
Understanding Special Tables: Some Things You Should Know by Dr. R.W. “Bill” Hamilton, 1992
The Trimix Report: A Look at the First 1500-2000 Tech Trimix Dives by Michael Menduno, 1993
Key West Consortium Trimix Tables
Is The Market Ready For Mix?
by Michael Menduno
This editorial was originally published in aquaCORPS: The Journal for Technical Diving #4 MIX, January 1992
“The best way to predict the future is to invent it. This is the century to be proactive about the future.” Alan C. Kay, Stanford Computer Forum 1987
There was a time not long ago that “AIR” was rarely thought of as a gas in sport diving circles, much less a technology. Like the old adage regarding a fish’s description of water, “AIR” was simply what we breathed and diving was no exception. Now it seems that the whole concept of “air technology”—a single gas to handle all exposures—may be out-moded before most of us knew enough to call it nitrox. What’s going on?

The self-contained diving market is in the midst of a technological revolution that is changing the way we think about diving. Similar to the PC in the world of computing, technologies and methods once limited to commercial and military use including: special mixed gases, more reliable decompression methods, diver propulsion vehicles, communications, closed circuit systems, and more, are now being rescaled and applied to sport and special interest diving, driven by the need for increased safety and performance.
Until recently, this community was viewed largely as a single, homogeneous group known as “recreational divers.” Now a more sophisticated view is emerging. To borrow several terms from the computer industry, the consumer diving market is in fact made up of many different user groups, each with its own specific diving environment and applications, and a need for appropriate tools. That’s what makes the technical revolution potentially so profound.
If the benefits of these technologies were limited to a few isolated high-tech divers, their impact would be relatively minor. Instead the tools, methods, and disciplines that are being pioneered today are applicable to a wide range of diving—from recreation to professional—and hold great promise for improving diver safety. The result is a significant opportunity for growth, and with it the need for caution and responsibility.
Conceived in the early 1900s, and developed and used in industrial and military operations over the last fifty years, mix technology offers the capability of reliably supporting divers to depths beyond 2000 fsw. At the same time, if used improperly or irresponsibly, it can be deadly. And that is cause for great concern. Though mix has been a long proven standard among its industrial and military counterparts, the sport diving industry has found challenge enough in teaching divers not to “run out of air,” let alone to manage alternative breathing mixtures. Mix technology may be ready for the market; the real question is, “Is the market ready for mix?”
Like the personal computer of ten years ago, special mix is being successfully utilized today by only a small number of experienced divers representing the vanguard of the field. We still have a long way to go before this technology can be reliably employed by the masses. Safety is the primary concern. Training and education, information, and a consistent set of operating guidelines are sorely needed at both industry and consumer levels, and there is a good deal of supporting infrastructure that is simply not in place.

With foresight, work, and the willingness to tackle the many hard issues that remain, mix technology, like the PC, will become accessible, reliable and easy to use, to the benefit of divers at all levels. Because, if kept in the closet or ignored, it will surely become a source of harm.
Now is a time for the industry to pull together, and chart a path for the future as we transition from a “fixed mix” to a multi-mix diving environment By being proactive, we stand to usher in a new era of diving, rivaling that initiated by the introduction of open circuit scuba nearly 50 years ago, and in doing so, we can make it a safer and richer activity for generations of divers to come. That’s what this issue of aquaCorps is all about.—M2
Understanding Special Tables: Some Things You Should Know
by Dr. R.W. “Bill” Hamilton
This article was originally published in aquaCORPS: The Journal for Technical Diving #4 MIX, January, 1992
Ever since the invention of a reliable means to supply compressed gas to divers, diving operations have been limited by the availability of appropriate decompression tables and methods. Now, with increased interest in alternative breathing mixes, advanced decompression methods, and exposures outside the range of standard air tables, special application tables are becoming an important tool in the high tech diver’s arsenal and are growing in use.

Conceptually, special tables are no different than their public domain counterparts. Each represents a decompression procedure designed to bring a diver back to the surface without incident after carrying out a planned exposure. Where public domain tables span an entire range of dives—for example 0-58 msw/0-190 fsw with bottom times ranging from five to several hundred minutes depending on the depth—and typically involve a single gas mix—usually air—special tables are typically calculated for a specific operation involving a narrow range of exposures, multiple gas mixes, decompression procedures, and custom J-factors (“Jesus” factors added for conservatism).
Another important difference: Though most public tables have been tested on a significant number of dives, this is not always the case with special tables for which limited diving data may exist—a reason to proceed with caution. Anyone with a computer and computational algorithm can generate a table. The real issue is what the numbers mean. As Dr. Bill Hamilton points out in the article below, special tables are only as good as the experience and judgement behind them. For that reason, decompression engineering is still as much of an art as it is a science.
“No matter what computational algorithm is used to produce a decompression table, it’s basis is still empirical. What works, works.” —RWH
Currently, special tables are being used by a small minority of technical divers, and there are only a few suppliers. For good reason—planning and conducting dives involving special tables requires a degree of skill, sophistication, and understanding that does not yet exist in the community as a whole. Training, experience, and a supporting infrastructure are required, and the potential for injury is no small matter. For that reason, many professionals in the field remain leery of producing tables for just anyone, particularly in light of the current legal climate in the industry. As special mix diving becomes more accessible, the need for special tables will continue to grow, and with it, the number of reliable suppliers. Until that time, it’s wise to proceed with caution and to work with qualified, experienced individuals who know what they’re doing. As Dr. Hamilton explains, there is a lot more involved than simply cutting a table.—Michael Menduno

Many of you have asked about the preparation of special application tables. This is a somewhat sensitive subject that raises many issues, and I think it worthwhile to discuss. One issue is whether professional diving physiologists and decompression consultants should support the extreme exposure diving that some people want to do. Another is whether a calculated table is reliable enough to keep the user out of trouble.

When I first began working with the technical diving community, I was approached by several divers who told me what they were planning to do, and it appeared they would make up the tables themselves if I could not provide them. Thus blackmailed, and having the humility at least to realize that some of the more experienced high tech divers could easily construct a table as well as I could, I went ahead with the project and generated a set of tables for them (with some trepidation, I might add). Fortunately, it has worked out well, and because of excellent feedback and sufficient repetition, I now am relatively comfortable with the process. Note, I do not view this business as “selling tables.” Rather, it is a professional service provided to clients that includes the generation of tables. As you will see, this involves much more.
Generating a special or custom table typically begins by finding out something about the client. The individual must be totally comfortable with gas and pressure physics and physiology, with oxygen safety as it applies to both the gas as well as understanding its physiological effects, and gas logistics and decompression methods, including the technical and operational aspects of the type of diving they’re doing.
The important thing to understand is that a reliable decompression table is not based on a formula alone. With today’s knowledge, no matter what computational algorithm is used to produce a decompression table, its basis is still empirical; tables are based on field experience, and (Ed. note: data!) “What works, works.” Although we have sophisticated computational methods—and they are getting better—there is a fair degree of judgement involved in incorporating the experience of yesterday’s dive into tomorrow’s table. For that reason, table development is still something of an art that extends beyond the ability to solve exponential gas loading equations.
The reason for this is the statistical nature of the process; it takes many, many dives to know anything at all about incidence rates inherent in a set of tables. For example, if an individual does five dives with no problems, this only means that at a 95% confidence level, the tables have a bends incidence [Ed.rate of decompression illness] of less than 50%. It takes literally hundreds of clean dives to be sure the incidence is less than 1%. Even a couple dozen clean dives should not be greeted with too much confidence. This is especially true if many of these are not conducted for the full time and depth.

To help mitigate this situation, the relatively new technique of applying maximum likelihood analysis to decompression makes it possible to estimate the risk involved with a given table based on a set of previous dives. In addition, guidelines have been developed for the development and validation of new and revised tables, and the ongoing management of existing ones (See “Validation of decompression tables.” Proceedings of the 37th Undersea and Hyperbaric Medical Society Workshop, Schreiner HR, Hamilton RW, editors. UHMS Publication 74(VAL)1-1-88. Bethesda, MA 1989). Under these guidelines, tables based on documented experience can be introduced at the “operational evaluation” stage if done with sufficient care.
The basic table computational methods used by most decompression consultants are still primarily Haldanian which uses compartments (commonly but inappropriately called “tissues”), exponential gas loading equations, and ascent constraints called M-values. Promising variations include bubble growth or bubble generation factors as well, but these too are usually fed by gas loadings. The Haldane method has its defects but is workable as long as one takes its weaknesses into account and stays sufficiently close to past experience i.e. what worked in the past. Personally, I prefer the “Haldane-Workman-Schreiner” method, which is a considerable advancement over Haldane.

Once a formula is decided upon, it is necessary to consider other factors involved in decompression management such as the range and variation of gas mixtures, particularly oxygen management; oxygen is the key to reliable decompression. The table should take into account the oxygen tolerance limits of the diver, both of their central nervous system (CNS) and “whole body.” The rates of travel and gas mix changes should be included in the table as instructions where they are needed, as well as the accumulated decompression time—or “decom time”—as well as the “stop time” at each stop. (For a discussion of decompression time management, see Decompression Strategies, M. Menduno, Technical Diver 2.2 , Summer 1990).

For technical dives, gas switches are usually determined by the specific dive plan. These are, of course, worked out in conjunction with the dive team. Once a basic operational approach is established for a dive, it is usually a relatively simple matter to make adjustments for the many factors involved, such as extensions of depth and time and J-factors, among others. However, to consider all of these, check the process thoroughly, and be sure the user has the right instructions are not trivial matters. For that reason, I feel it’s important to label tables and the corresponding computations with a unique traceable basecase name, and I encourage others to do the same rather than just calling a table the “DCAP 250/30″ or the “Wakulla tables.” That way, the origin of any table or computation can be traced and reviewed, an otherwise time-consuming task that can result in confusion.
Another important thing that I feel is necessary is to provide the user with instructions on how to use the tables. Although you obviously cannot tell the user everything they need to know in order to perform a sophisticated dive operation requiring special tables, it is important that creators include at least a description of every item on the table and how to use them. Finally, although it’s not something that can always be enforced, I feel it is important that clients agree to provide feedback as to the results of using a set of tables. The data we get from such feedback is valuable and allows us to continue to improve the methodology.
Generating special tables for a range where the parameters are familiar and there is sufficient available experience typically represents about a day’s work and can run anywhere from US $200-$500 and up depending on the supplier. More exotic tables, requiring the acquisition and analysis of specific data, take a good deal more time and thus can cost a great deal more (often a couple of orders of magnitude more for the development of a full set of commercial or professional tables). Note that the time it takes may bear very little relation to the value of the table, but it does have an impact on the cost.

No table or decompression method is completely “safe.” In fact, I do not even use that word in conjunction with decompression. It’s wrong on several counts. First, no significant dive is free of the risk of decompression sickness. Second, DCS is not an accident; it happens and it will continue to happen as a predictable part of diving.
The dive team should plan for it, and in doing so can reduce the consequences to as near zero as possible. When DCS does occur, it can and should be treated promptly and adequately and, if this is done, the chance of residual injury is quite small.
First, no significant dive is free of the risk of decompression sickness. Second, DCS is not an accident; it happens and it will continue to happen as a predictable part of diving. The dive team should plan for it, and in doing so can reduce the consequences to as near zero as possible.
The real accidents that take divers’ lives are due to operational problems like running out of gas, getting lost or entangled, not pushing a dive computer, or running over a table. In my opinion, this is where some current technical diving practices seem to be operationally inadequate. Technical dives are operations. As such, they should have a leader and/or safety manager, planning, cooperation, and the predetermined ability to cope when any step falls short.

This means building in redundancy throughout: in equipment, extra gas for contingencies, extra oxygen on board, and ensuring that other team members, especially the boat captain, know what’s going on and what to do if things don’t go as planned. Having understanding and agreements before the fact can go a long way to allay the consequences of a glitch in the operation.
Technical diving can also be risky. The divers assume this risk, fully and personally, but this does not justify taking unnecessary risks. Tricks like diving on air to 89 m/290 ft are selfish and irresponsible. The diver who does not get away with this may be the only one to die but will not be the only one to suffer. Accidents reflect on all divers and can set progress back in a variety of ways. If you want to keep pushing the envelope, fine, but do it intelligently with care and responsibility.
The decision to use special tables depends on the specific operational plan for the dive, whether special breathing mixtures or accelerated decompression methods are to be used, and whether or not a general purpose table is applicable. Whatever your decision, make sure that the tables you’re planning to use were generated by a reputable supplier and are, in fact, appropriate for the dives you’re planning to do. It goes without saying that you should have the necessary experience, training, and equipment required for the operation in question. No matter how reliable, no table can make up for lack of judgement or the inability of the diver to carry it out.

Dive Deeper:
InDepth: Dr. Bill Talks Mix: The late great decompression physiologist, Dr. R. W. “Bill” Hamilton played a unique role in the early development and emergence of technical diving. Listen to “Dr. Bill” and cave diver nurse anesthetist John Crea discuss “special mix” diving at the TEK.95 conference (1995).
aquaCORPS #1 UnderPressure: “Call It High Tech Diving,” by RW Bill Hamilton, 1990
X-Ray: In Memoriam: Joel Silverstein’s The Prince of Gases: RW “Bill Hamilton (1930-2011) in X-Ray magazine.
The Trimix Report
by Michael Menduno.
This article was originally published in aquaCORPS: The Journal for Technical Diving #6 COMPUTING, June 1993

Though trimix is being used successfully by small groups of divers in the U.K., Mexico, France, and Switzerland, most of the current work is being done in America. To date, conservatively 1,500-2,000 open circuit trimix dives have been conducted in the U.S. since 1987 by divers from the wreck, cave, and scientific diving communities. Depths range from about 46-267 msw/150-870 fsw, though the majority of these dives have been conducted in the 61-107 msw/200-350 fsw range with typical bottom times of 20-30 minutes, ranging up to 60 minutes. Approximately 100 dives have been conducted in the 92-153 msw/300-500 fsw range and only a handful in excess of 153 msw/500 fsw. These have been conducted by several leading cave explorers including Sheck Exley, US; Jim King, US; Claude Toulomdjian, France; and Jochen Hassenmayer, Switzerland.

Dr. R.W. Bill Hamilton of Hamilton Research Ltd, Tarrytown, NY, has been responsible for developing decompression procedures for a large number of these dives using his Diving Computational Analysis Program (DCAP) computational algorithm. Schedules from John Crea, Submariner Research Ltd., Bainbridge, GA; Randy Bohrer, Underwater Applications Corp, Nashua, NH; Kevin Gurr, Aquatronics, Redding, UK; and other sources were used as well. To date, the decompression experience has been good. In four reported incidents, two were “suspected” decompression illness (DCI) and were successfully treated with surface oxygen following the dive. Another possible DCI incident appears to have involved minor pain-only symptoms that were resolved without chamber treatment, an option that was refused by the diver. A final, apparently mild, DCI incident occurred following a 20 minute, 92 msw/300 fsw exposure and was treated successfully with a USN Table 5.
With regard to operational safety, three fatalities, one “near miss,” and a “blow-up” resulting in decompression illness occurred during trimix diving operations in the US in the last two years, although these had little to do with the gas mix itself. The first fatality was due to a freak water reversal in an underwater cave near Tallahassee, Florida, that resulted in two divers being trapped during a deep mix dive. One member of the team survived. The second fatality occurred on the Andrea Doria, when a diver who had separated from his partner during a wreck penetration run, ran out of gas after exiting, and drowned. Several weeks later, another fatality, when a diver got lost in the wreck after getting separated from the team’s mainline during a trimix operation and drowned. In another incident, related to mix, a diver suffered a CNS convulsion during in-water oxygen decompression following a deep mix dive when he lost buoyancy control, drifted down, and “dozed off” at 11 msw/35 fsw (PO2=2.1). The diver, a paramedic, had had only two hours of sleep the night before the dive. Managing to inflate his BCD before convulsing, he floated to the surface, and was rescued by an excellent surface support team and resuscitated. A final incident was due to operational problems during a wreck dive—the diver missed the “down line” on descent, got lost, ran out of gas, and was forced to “blow up” to the surface omitting decompression. He was rescued, evacuated to a chamber and treated successfully.1
1See “Safety First, An Analysis of Recent Diving Accidents,” by Michael Menduno, technicalDIVER 3.2, 1992, pg.23.
Methods, Procedures and Training

From a technological perspective, a focus of many of these pioneering dives has been to develop reliable operational procedures including gas mixes, reliable decompression methods, staging, and adequate diver support. Two groups, led by Capt. Billy Deans of Key West Diver Inc., Key West, Florida; Jim King of Deep Breathing Systems, Sevierville, Tennessee; and several other individuals, including Sheck Exley, have been responsible for much of this effort in the U.S. Their work draws on the earlier work of the Wakulla Project conceived and led by Dr. Bill Stone (“The Wakulla Springs Project,” edited by Dr.William C. Stone, U.S. Deep Cave Diving team , Derwood , MD.1989); the Sullivan Connection project organized by Bill Gavin, Bill Main, and Parker Turner; and Sheck Exley’s pioneering dives. Open water work utilizing heliox mixes has also been conducted by Ken Clayton, Washington D.C.; Gary Gentile, Philadelphia, Pennsylvania; and Steve Gatto, Atco, New Jersey.
Key West Diver has developed many of the field methods and procedures for open water operations and has served as a training center for the majority of other technical diving operators and many users in the US and abroad (Presently there are about ten operators/user groups regularly conducting trimix diving operations and offering training—see below). In parallel, Deep Breathing Systems has been responsible for developing many of the operational procedures and equipment for deeper exploration work. In addition, with the help of Canada’s Defence and Civil Institute of Environmental Medicine (DCIEM) Toronto, Canada, Deep Breathing Systems has spearheaded the testing and validation of the decompression methods and tables generated by the DCAP algorithm using Doppler monitoring and other tests designed to measure decompression stress.

On the training side, the International Association of Nitrox and Technical Divers (IANTD), Miami, Florida, led by Tom Mount, has pioneered the development of user and instructor trimix training programs and currently has a roster of over 20 trimix instructors (see the tek.GUIDE, aquaCorps Journal #5, 1993, for facility and instructor listings). IANTD has made significant progress over the last year in developing training standards, texts, and materials with the help of Dr. Lee Somers, University of Michigan, Ann Arbor, Michigan, and is currently the only company offering formal trimix certification.
[Ed. note—American Nitrox Divers Inc (ANDI), Professional Scuba Instructors Intl (PSAI) Technical Diving International (TDI) followed within two years.]


IANTD has reportedly just obtained instructor insurance to cover its activities, though rates are not yet available. Island Scuba Center, headquarters of ANDI, has been conducting trimix dives for some time and plans to launch an extended range program later this year. In addition, there is at least one University trimix diving program at Florida State University that was developed by Gregg Stanton. The British are also involved through IANTD UK, Somerset, England, headed by Rob Palmer, though their efforts to date have focused primarily on enriched air nitrox and some of the early development work on closed circuit rebreathers. There is also some interest in Australia, spearheaded by Rob Cason—an IANTD director—of Fun Dive Centre, Sidney, NSW, and others.
Operating Guidelines

Though rudimentary training standards exist, there is as yet no written set of operating guidelines for self-contained trimix diving. However, an emerging set of “community” operational guidelines is developing with some success. (See “Blueprint for Survival Revisited”). With regard to deep diving, the emerging “community consensus” is that dives beyond about 62 msw/200 fsw should be conducted on a helium-based mix.
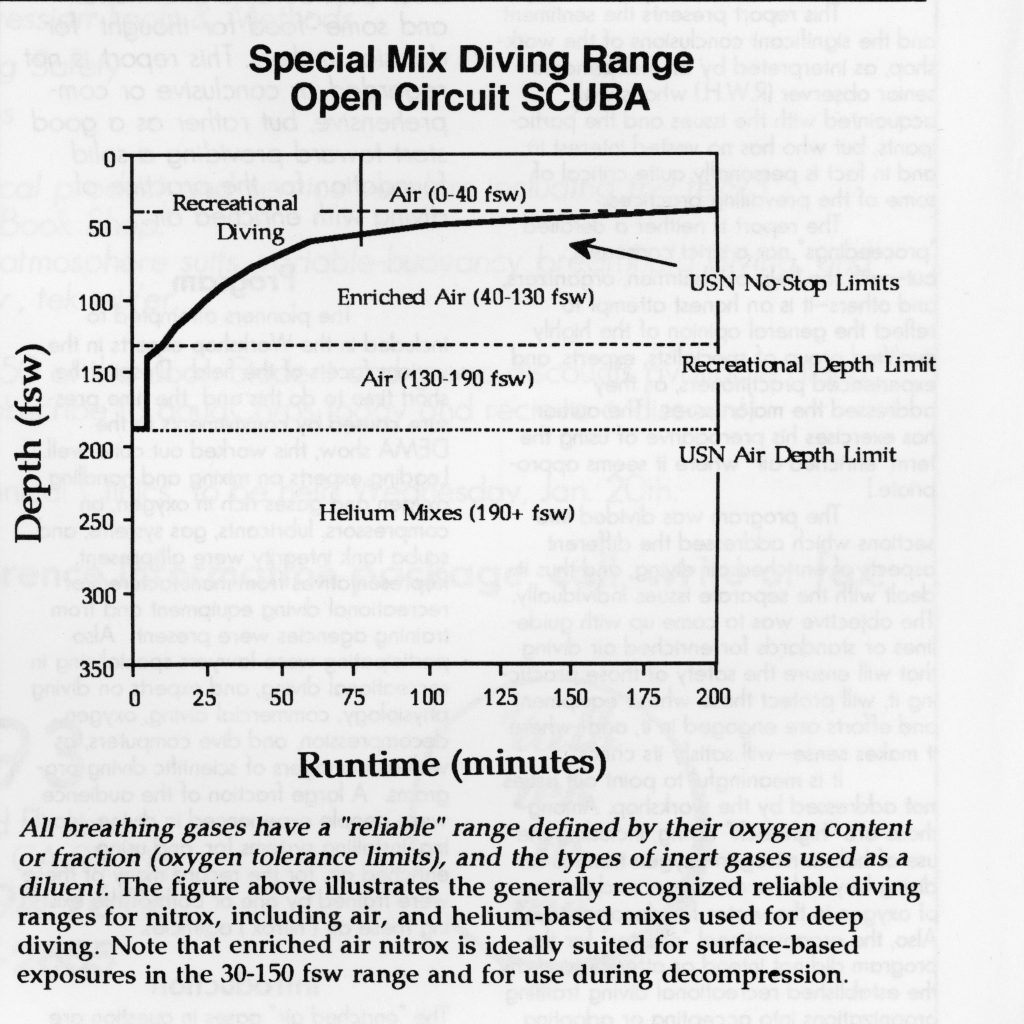
Today, most U.S. dives conducted in the 55-92 msw/180-300 fsw range have standardized around the use of trimix 14-17/X, (14-17% FO2 depending on the depth, FHe=25-60%, maximum working PO2= 1.4-1.45 atm) with an “equivalent narcotic depth” (END) ranging from 26-54 msw/85-175 fsw depending on the exposure and application. Though “lean” trimixes with a helium content of 25% or less (an END of 54 m/175 f at 76 msw/250 fsw)—sometimes referred to as “poor person’s mix” or heliair (helium-diluted air) on the basis of their relatively low cost and mixing ease—are sometimes used to reduce the risk of O2 toxicity and “take the edge off narcosis,” the general thinking today is to eliminate as much narcosis as is economically feasible.
As a result, mixes with at least 50% helium (an END of 26-36 msw/85-118 fsw at depths of 76-92 msw/250-300 fsw) are gaining in popularity and will likely become a community standard. Decompressions for these operations utilize a single enriched air nitrox (EAN) intermediate mix, typically an EAN 32-36, which is breathed beginning at the first or early decompression stops—typically in the 33-40 msw/110-130 fsw range—followed by oxygen breathing at the 3 and 6 msw/10 and 20 fsw stops. Based on the success of these procedures, a set of provisionally-standardized trimix decompression schedules for dives to 76 msw/250 fsw, known as the “Key West Consortium Tables” (see below), were prepared by Key West Diver and Hamilton Research Ltd, to assist in standardizing operations and managing access to tables.


These tables are unique in that they allow a “variable percentage of helium,” and have been adopted by the majority of technical diving operators in the US, including Enchanted Diver, Floral Park, NY; The Gas Station, Gloucester, NJ; Ocean Odyssey, Santa Cruz, CA; and Scuba Adventures, San Bernardino, CA. Schedules utilizing air as an intermediate gas were also developed by Underwater Applications Corp. and used with success where access to sufficient onboard enriched air nitrox supplies is a problem.
For deeper dives in 92-153 msw/300-500 fsw, ENDs are generally set at 46 msw/150 fsw or less, and decompression procedures typically involve air as an intermediate gas beginning as deep as 67-70 msw/220-230 fsw, followed by one or more enriched air intermediate mixes. For example, a typical procedure is to use an EAN 30 for stops beginning at 46 msw/150 fsw with a switch to EAN 46-50 at the 24-21 msw/80-70 fsw stops. This would be followed by oxygen decompression at 6-9 msw/20-30 fsw. (Ed. note—the community consensus is to limit oxygen use to 6 msw/20 fsw or less.) Doppler testing following these dives has suggested the use of air as a deep intermediate gas reduces decompression stress significantly, though the jolt of “instant” narcosis and cumulative oxygen tolerance must be managed with care.




In response to the desire to maximize dive time at remote sites—for example, during offshore wreck diving operations—provisional repetitive trimix decompression procedures were prepared by Hamilton Research Ltd. utilizing conventional gas loading analysis. This method is criticized by some experts, but there is no accepted computational algorithm for repetitive diving. Though the potential for being able to employ repetitive diving seems promising and will probably grow as trimix use becomes more widespread within the community, these tables have received only minor usage to date. More data is needed in order to refine the computational method. Work on altitude tables has also been done by Submariner Research Ltd. and Underwater Applications Corporation for specific applications.
The next boom in decompression management tools will likely come from the growth of “desktop decompression software”—computational algorithms running on a personal computer being pioneered by Corey Bergren of Cybertronix, Knoxville, Tennessee; Sheck Exley, Dr. X, Live Oak, Florida; Kevin Gurr, Aquatronics, Redding, England; and Dan Nafe, Miami, Florida.
The Operations Approach

To date, the field experience with trimix has shown that a rigorous “operations approach,” including thorough planning, proper equipment, diver support, competent execution, and the ability to respond promptly to and deal effectively with emergencies, is required to conduct these dives safely. Deep mix dives are by their nature complex because of the gas, decompression, and equipment management involved. Much can potentially go wrong. Simply breathing a mix is the easy part. The general consensus seems to be that the community still has a long way to go in improving operational procedures. In this respect, a lot can no doubt be learned from the commercial diving community.
Over the next five years, trimix diving—supported by an “operations approach” and more in depth training—is expected to grow and become more accessible because of its safety advantages. As a result, trimix/heliox will likely replace the use of air for open circuit deep diving operations beyond about 55 msw/180 fsw— that is, until reliable, low-cost, closed circuit systems find their way to market. Take another breath!
Key West Consortium Trimix Tables
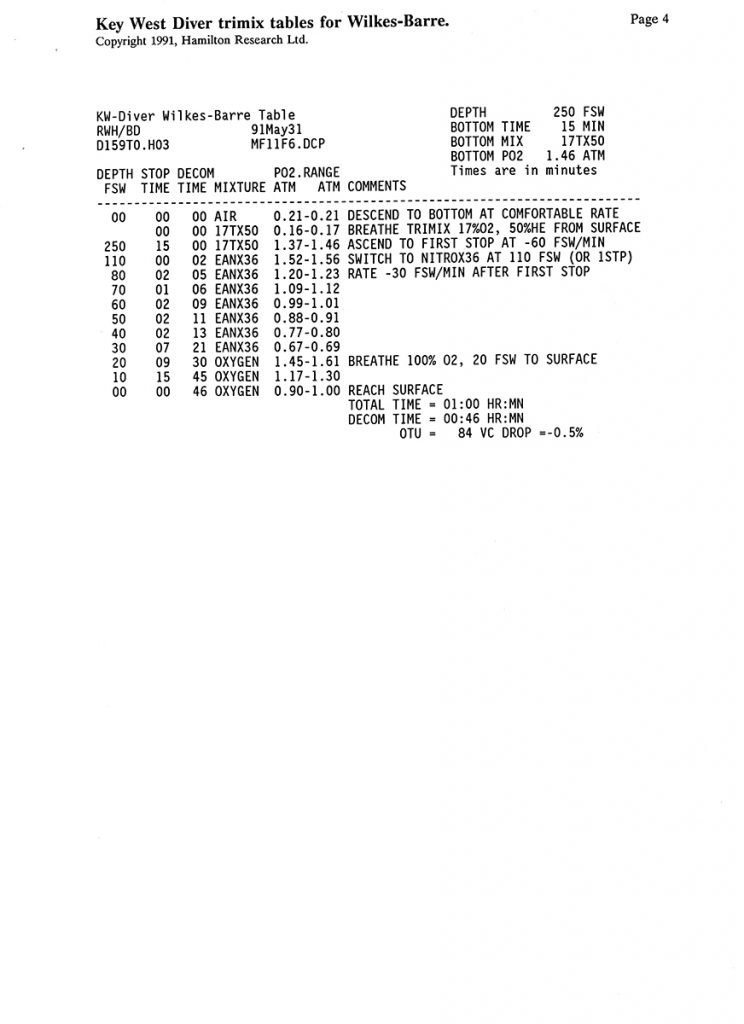
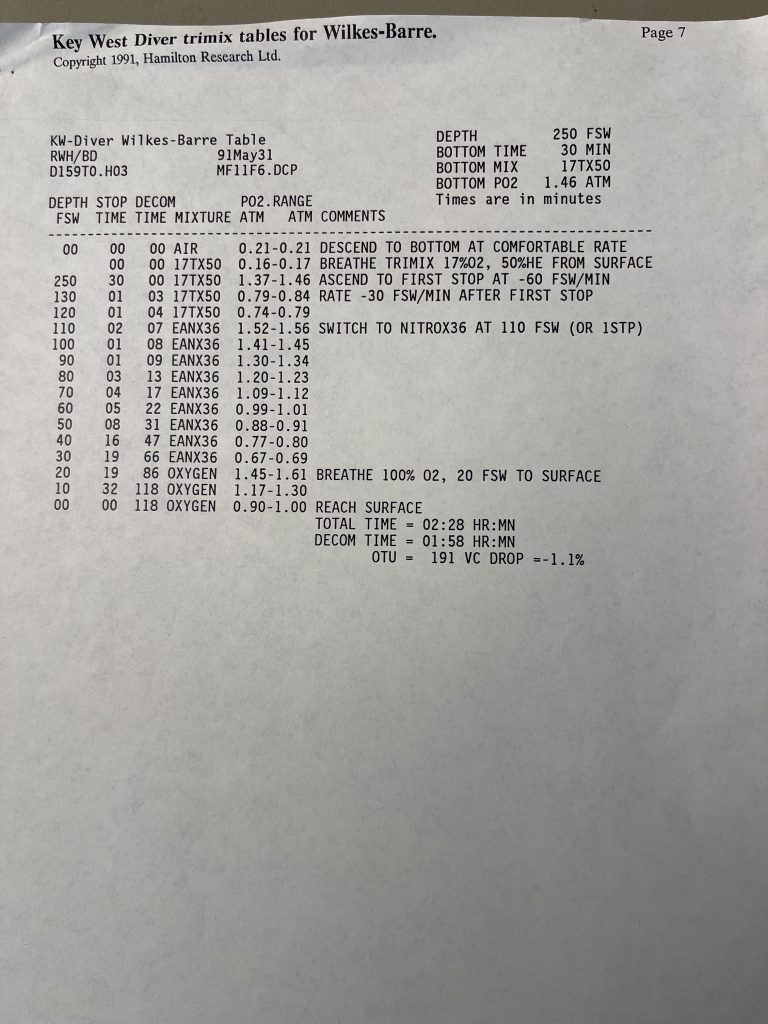
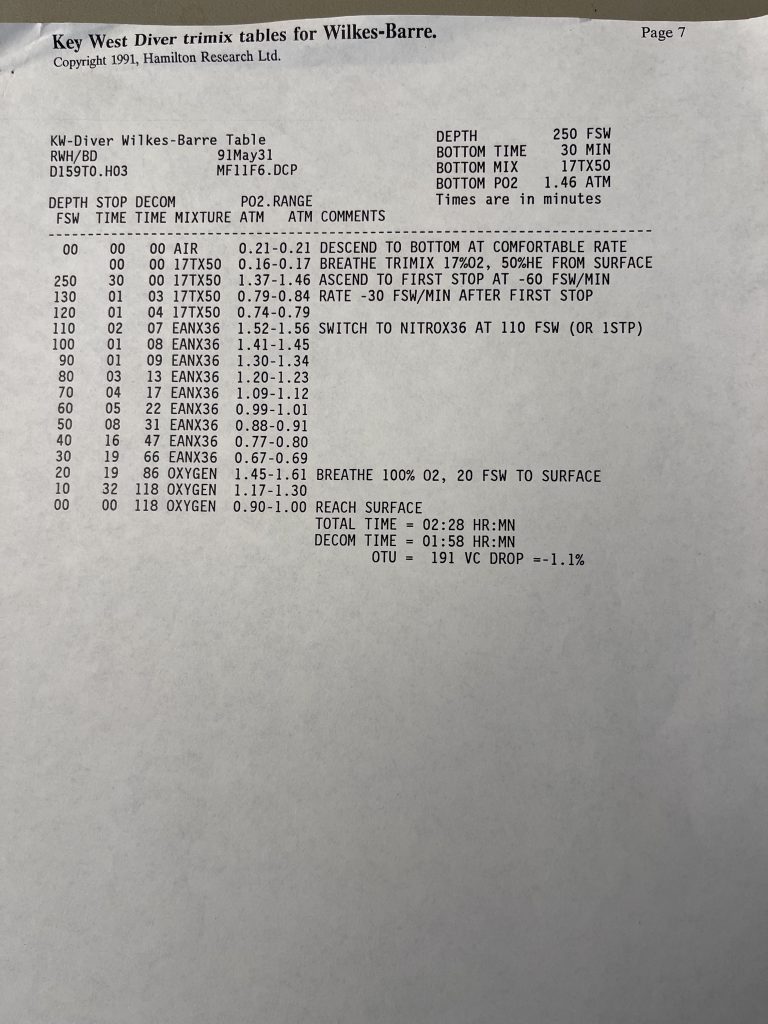
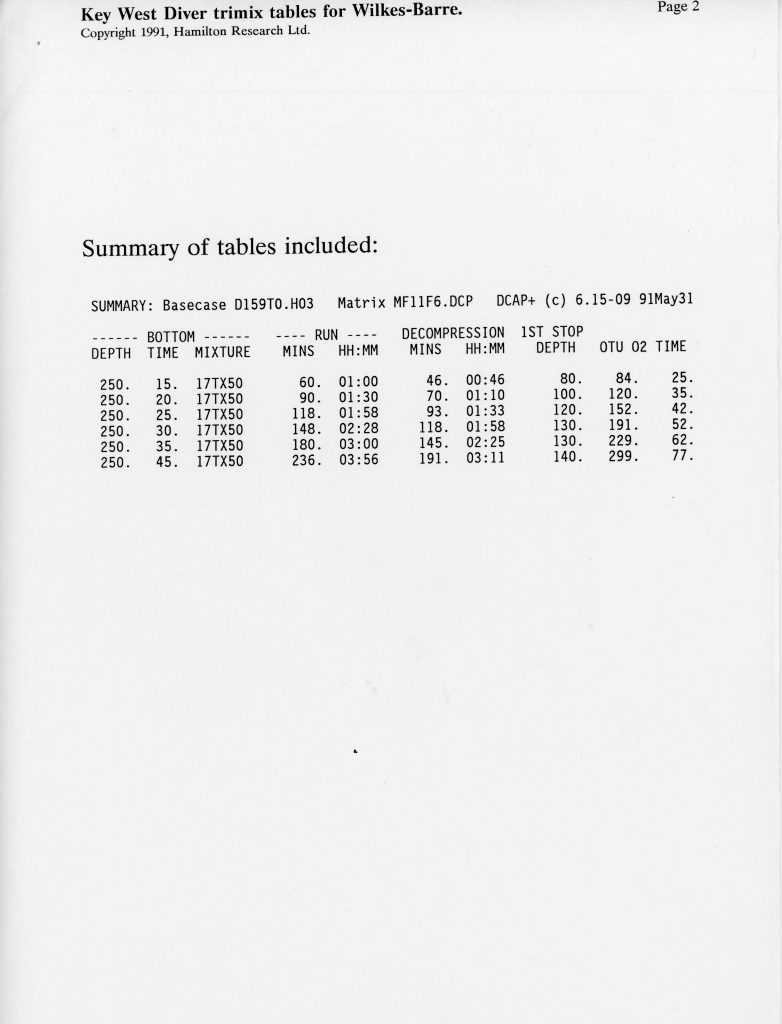
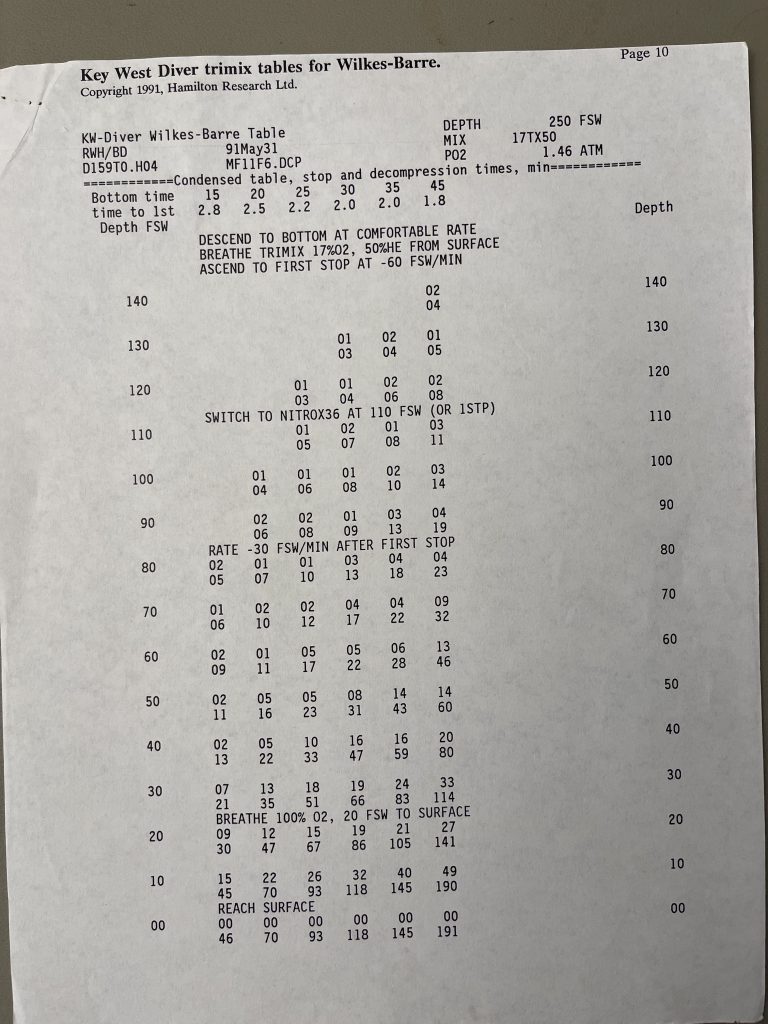
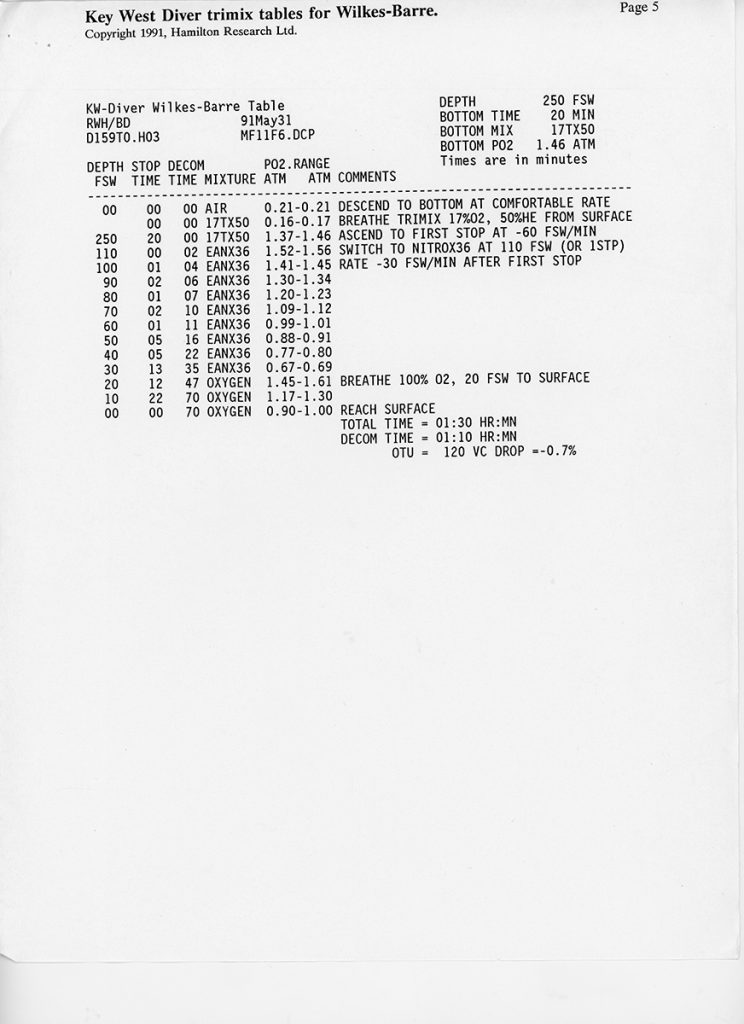
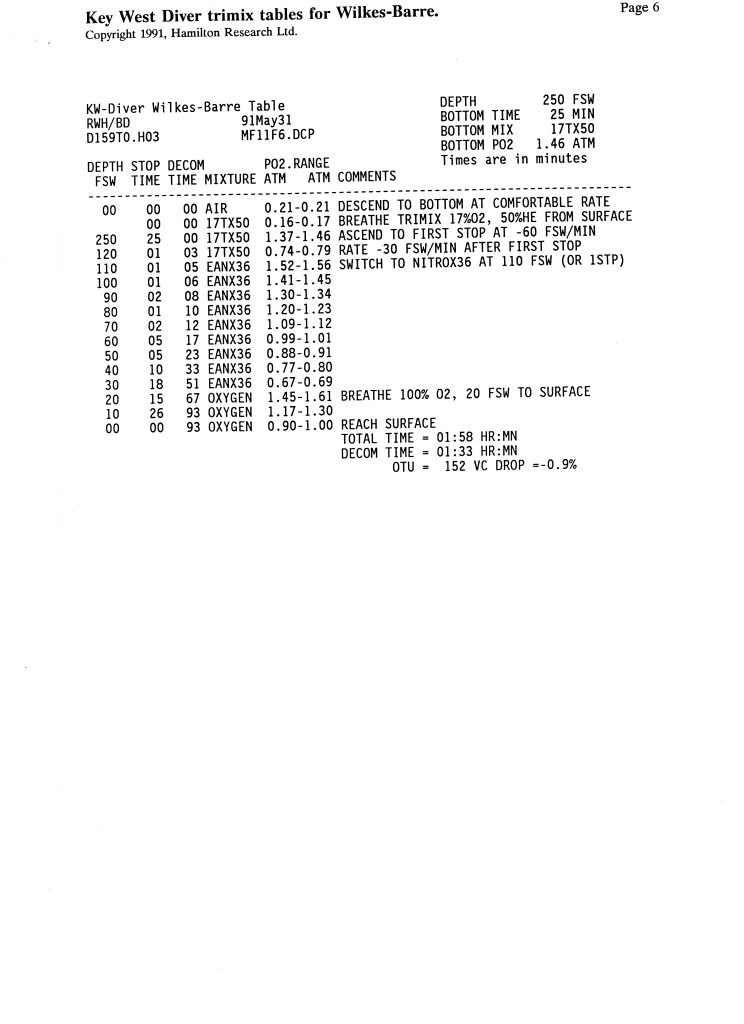
Trimix, or as it then was called, “special mix diving,” required tables or a program to generate them. There were no dive computers at the time that calculated deco for mixes other than nitrox. A group of technical divers including Billy Deans, Lou Sarlo, Bart Malone and Jennifer Hunt pitched in to purchase a set of trimix tables from Bill Hamilton for diving depths of 190-250 fsw/58-76 m with varying bottom times, and with helium fractions from 17%-50% They were known as the “Key West Consortium Tables.” Here is a selection for dives to 250 fsw/76 msw with 10-45 minute bottom times and a set of reset tables as well.—M2.








Dive Deeper:

Michael Menduno/M2 is InDepth’s editor-in-chief and an award-winning journalist and technologist who has written about diving and diving technology for more than 30 years. He coined the term “technical diving.” His magazine “aquaCORPS: The Journal for Technical Diving” (1990-1996) helped usher tech diving into mainstream sports diving, and he produced the first tek.Conferences and Rebreather Forums 1.0 & 2.0. In addition to InDepth, Menduno serves as an editor/reporter for DAN Europe’s Alert Diver magazine, a contributing editor for X-Ray mag, and writes for DeeperBlue.com. He is on the board of the Historical Diving Society (USA), and a member of the Rebreather Training Council.

Dr. R.W. Bill Hamilton (1930-2011) is a diving physiologist and principal of Hamilton Research Ltd. with over 20 years of decompression management experience in the hyperbaric and aerospace industries.
Be A Part of History: To access our treasure trove of dive history and become a member, visit us at: www.HDS.org. We are also on Facebook: Historical Diving Society USA






















































